Hi Friends,
On Tuesday I flew to Palm Springs for my follow-up CT scan to see whether the PEF lung ablation I had in January was successful.
Because I had a full-blown anaphylactic reaction to the contrast from the brain MRI two weeks ago, they had to take special precautions and premedicate me with three drugs. They explained that since I reacted to MRI contrast, I’m now considered at higher risk for reacting to CT contrast as well. Lucky me.
The interesting thing is that I’ve had more imaging in the last three years (CT scans, MRIs, PET scans) than Imelda Marcos had shoes… and I had never reacted before, let alone with anaphylaxis.
But almost immediately after the contrast was injected during the MRI, I got a crushing headache, started vomiting, my blood pressure skyrocketed, I began wheezing, and broke out in hives. They stopped the scan, called the doctor, and skipped the second half because the contrast had worn off and they didn’t want to give me any more.
After an experience like that, you really don’t feel eager to have another scan—especially with contrast. But I needed answers, so I agreed to one more CT with contrast. I went into it with much more apprehension than usual.
Especially since starting IVs on me is so hard. I’ve been poked more times than a snoring husband who refuses to wear his CPAP machine. Perhaps it wouldn’t be so bad if they could actually find my veins the first time. I feel like a human pincushion. Honestly, voodoo dolls get poked less than I do. 🤣
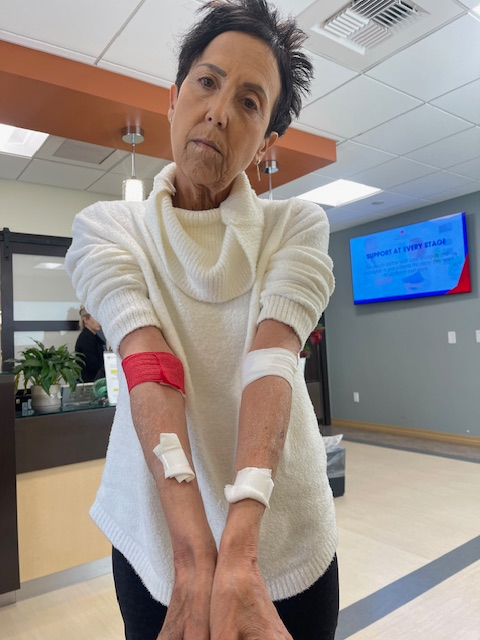
After four attempts to start an IV, I said ENOUGH and demanded an RN from the VAT Team (Vascular Access Team). With her confidence and experience, Jennifer found a vein on the first painless puncture and never even needed the ultrasound to locate it.
Wednesday marked exactly three years since I was diagnosed with lung cancer.
It was also the day I met with Dr. Thomas at Eisenhower Health to review the results of my ablation.
Drum roll, please…
The doctor came into the room with a smile on his face and said he had good news.
He said the two metastases I had in my bronchial lymph nodes were essentially gone, which means a complete response.
The fact that the primary tumor—which had grown on every CT scan over the past three years—has now stopped growing and is stable means I achieved a partial response.
He said he would like to repeat the PEF ablation in six weeks using a new and more powerful machine.
And my anesthesia angel, Dr. Michael Kessler, will be back in the OR with him.
Tomorrow I’ll see Dr. Myall, my oncologist at Stanford Health Care, who will review the results of my recent brain MRI and PET scan.
He told me the brain MRI without contrast is incomplete, but frankly, I do not want that contrast injected into me again—premedicated or not.
I’ll also meet with a genetics doctor to help make sense of some of the mutations discovered in my recent biopsies.
I promise to give you a full report next week on both visits.
And after that, I’d love to spend more time talking about all the fun things I love in life—dogs, dessert, improv, trivia, and all the recipes I’ve been creating for my community.
Until next week, I’m just going to keep believing in miracles.

Thank you all for your Love 💕 & Prayers 🙏.
Love and Benadryl,
Chef AJ